Clinical aspects of pelvic congestion syndrome
George GEROULAKOS2;
Mamuka BOKUCHAVA3
Claudia, Rome, Italy
2 Consultant Vascular Surgeon,
Department of Surgery, Charing Cross
Hospital, London, UK
3 Deputy Director of the Center of Vascular
and Heart Diseases, Tbilisi, Georgia
Abstract
The main symptom of pelvic congestion syndrome (PCS) is pelvic pain. Women typically have a dull, throbbing, and achy pain in the vulvar region, which often worsens during or after intercourse, just before the onset of menstruation, and as the day progresses, especially in women who stand or sit for long periods. The cause of PCS is unknown; however, multiple factors, such as venous reflux, venous obstruction, and hormones, are most likely involved. Pelvic pain and refluxing pelvic veins are often present in premenopausal women; however, their presence does not always establish a cause and effect relationship. In patients who have clinical symptoms, signs, and imaging findings compatible with PCS, the diagnosis can be made only after other causes of abdominal and pelvic pain have been excluded. The patient history should include the nature, intensity, pattern, location, duration, and radiation of the pain, as well as any exacerbating and relieving factors. PCS is more often diagnosed in multiparous women younger than 45 years old, possibly because the ovarian veins increase in size during each pregnancy and do not return to normal in women with PCS. The differential diagnoses for pelvic pain are vast, further adding to the complexity of the disorder.
Introduction
Signs and symptoms
Women with pelvic congestion syndrome (PCS) typically experience a constant dull and aching pain, but the pain is occasionally more acute. The pain is worse at the end of the day, during or after sexual intercourse, just before the onset of menstruation, and after long periods of standing or sitting; relief occurs when the patients lay down.1-6 Chronic pelvic pain can be debilitating, and it accounts for 10% to 15% of all visits to the gynecologist.2,6 Hemorrhoids and varicose veins of the perineum, buttocks, or lower extremities may also be present. Ovarian point tenderness during an examination in patients with a history of postcoital pain is sensitive and specific for PCS in 94% and 77% of cases, respectively.3 Other symptoms and signs include dysmenorrhea, back pain, vaginal discharge, abdominal bloating, mood swings, depression, and fatigue.4
Pregnancy
PCS is more often diagnosed in multiparous women younger than 45 years old, possibly because the ovarian veins increase in size during each pregnancy and, in women with PCS, the veins do not return to normal. PCS is rarely diagnosed in nulliparous women, and it has not been reported in postmenopausal women. In addition, women with PCS have a larger uterus and a thicker endometrium than women without PCS, and, in 56% of women, there are cystic changes that occur to the ovaries.3 Often, symptoms do not appear until a woman becomes pregnant, and then they continue after the pregnancy.
Vulvar varices
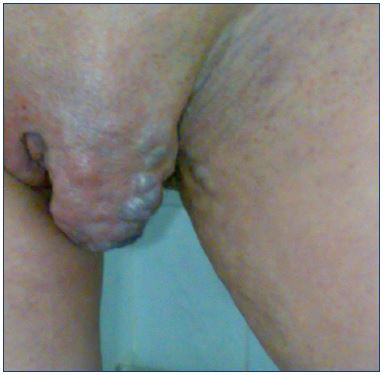
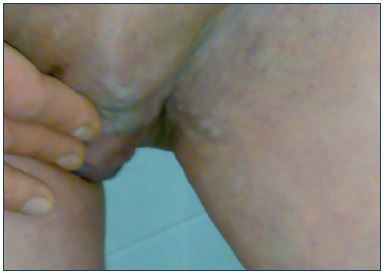
Vulvar varices occur in about 10% of pregnant women, but typically not during the first pregnancy. Generally, vulvar varices develop during month 5 of the second pregnancy. The risk increases with the number of pregnancies. The incidence of vulvar varices is underestimated because the varices are often asymptomatic; women may be embarrassed to talk about the problem; and doctors are not actively looking for varices when the patient is in a standing position during the physical examination at month 6 of pregnancy or during the first month after delivery. Vulvar varicosities tend to disappear spontaneously after delivery and rarely persist after 1 month.7 The typical PCS patient may or may not have vulvar varicosities, but they often have varicose veins. The varicosities usually extend along the medial aspect of the medial to posterior upper thigh and along the buttocks (Figures 1, 2, and 3).
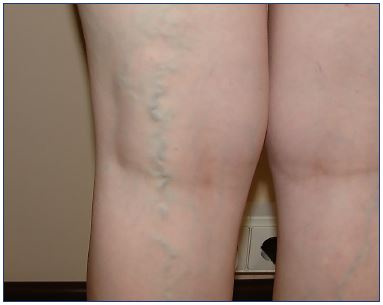
Figure 1. Varicose veins in a patient with pelvic congestion
syndrome.
The left leg is presenting more than the right.
Causes of PCS
The cause of PCS is unknown; however, multiple factors, such as venous reflux, venous obstruction, and hormones, are most likely involved. Incompetent and dilated pelvic veins are common, and, according to the literature, 10% of the female population has ovarian varices. Pelvic pain and refluxing pelvic veins are often present in premenopausal women; however, their presence does not always establish a cause and effect relationship.
Patient evaluation
A detailed history and comprehensive examination are of paramount importance. The patient history should include the nature, intensity, pattern, location, duration, and radiation of the pain, as well as any exacerbating and relieving factors. The relationship between the pain and a woman’s menstrual cycle should be discussed. Women with depression, personality disorders, and domestic violence have a higher incidence of somatic complaints, and they should seek treatment from a trained mentalhealth professional. The discussion about patient history should involve a thorough discussion on the patient’s sleep patterns, lifestyle (eg, does the pain affect daily activities?), menstrual pattern, dyspareunia, urologic dysfunction, and any other gynecological issues. Irritable bowel syndrome has been reported in 65% to 79% of women with chronic pelvic pain. All previous consultations and diagnostic or therapeutic interventions should be discussed.
The physical examination should evaluate the varicose vein network, which may be present on the perineal, vulval, gluteal, or posterior thigh areas. According to Monedero et al, vulval varicosities develop due to reflux in the left and right ovarian and pudendal-obturator veins in the case of pelvic floor insufficiency; whereas, perineal, gluteal, and posterior thigh varicosities are mostly due to reflux in the internal iliac vein.8 In addition to an abdominal and pelvic examination, a thorough physical should include an examination of the neurological (evaluating the thoracolumbar spine), cardiovascular, pulmonary, and vascular (evidence of varicosities in the lower pelvis, buttocks, and legs) systems. Further testing should include a complete blood count, metabolic profile, urinalysis, and an endocervical swab for chlamydia.
Differential diagnoses
The main symptom of PCS is pelvic pain, but PCS is not easy to diagnose. Symptoms must be present for at least 6 months before a diagnosis of PCS can be considered.6 The differential diagnoses for pelvic pain are vast, further adding to the complexity of the disorder. These diagnoses include endometriosis, chronic pelvic inflammatory disease, leiomyoma, adenomyosis, Nutcracker syndrome, diverticulitis, diverticulosis, Meckel’s diverticulum, interstitial cystitis, abnormal bladder function, chronic urethritis, fasciitis, nerve entrapment syndrome, hernia, scoliosis, spondylolisthesis, osteitis pubis, somatization, psychosexual dysfunction, and depression. The diagnosis of pelvic congestion syndrome can only be made by excluding other causes of chronic pelvic pain, and managing this complex condition can be a challenge for the primary-care provider.
REFERENCES
1. Ignacio EA, Dua R, Sarin S, et al. Pelvic congestion syndrome: diagnosis and treatment. Semin Intervent Radiol. 2008;25:361-368.
2. Giacchetto C, Catizone F, Cotroneo GB, et al. Radiologic anatomy of the genital venous system in female patients with varicocele. Surg Gynecol Obstet. 1989;169:403-407.
3. Beard RW, Reginald PW, Wadsworth J. Clinical features of women with chronic lower abdominal pain and pelvic congestion. Br J Obstet Gynaecol. 1988;95:153-161.
4. Kim HS, Malhotra AD, Rowe PC, Lee JM, Venbrux AC. Embolotherapy for pelvic congestion syndrome: long-term results. J Vasc Interv Radiol. 2006;17:289-297.
5. Walling MK, Reiter RC, O’Hara MW, Milburn AK, Lilly G, Vincent SD. Abuse history and chronic pain in women: I. Prevalences of sexual abuse and physical abuse. Obstet Gynecol. 1994;84:193-199.
6. Allegra C, Antignani PL, Kalodiki E. News in Phlebology. Torino, Italy: Minerva Medica; 2013.
7. Van Cleef JF. Treatment of vulvar and perineal varicose veins. Phlebolymphology. 2011;18(1):38-43.
8. Monedero JL. Insuficiencia Venosa Cronica dela Pelvis y de los Miembros Inferiors. Madrid, Spain: Mosby/Doyma Libros SA; 1997