History of venous surgery (2)
This is the second of the 3 chapters that make up a “History of Venous Surgery”. In the latest
issue of Phlebolymphology (Vol. 18, No. 3, 2011), an overview from the ancient Egyptians to the
19th century was presented. In the present issue, the history continues with the 20th century.
Michel PERRIN
THE 20TH CENTURY
By the 20th century, venous surgery was no longer limited to treatment of varicose veins and had gradually expanded to include management of other venous diseases and treatment of veins other than superficial ones. We will successively describe varicose vein surgery and then other procedures.
VARICOSE VEIN SURGERY
A. Open surgical excision
With the exception of the highly disfiguring Rindfleisch operation of the early 20th century (1908), modern surgery for varicose veins based on their removal began at this time. An explanation is required as a reminder of the principle on which treatment of varicose veins is based by removal without preservation of the saphenous trunks. It is based on 2 concepts:
• First, a general concept: open surgery was most often limited to resection or removal of diseased organs or tissues insofar as their removal did not result in an excessive mortality rate or complications and subsequently enabled patient survival under acceptable conditions. Insofar as the superficial veins are not essential to return blood to the heart, because of the decisive role of the deep veins for this purpose, their removal was possible.
• The second concept is specific to varicose veins. It was considered that the progression of varicose veins over time occurred “from the upper area downward”, that is from the groin to the ankle. In other words, doctors were convinced that venous disease originated at the saphenous junction and increasingly extended towards the foot via the saphenous veins and their tributaries. Consequently, traditional open surgery consisted of ligation of the saphenous junction, and more or less extensive resection of the saphenous veins and of diseased tributaries. Since it was considered that the first incompetent valve was the last saphenous valve, ligation of the saphenous vein had to be performed on a level even with the deep vein.
What was going to change was the technique used for removal of the saphenous trunk, which we have seen had been used for hundreds of years. The venous stripping procedure for its removal was also destined to change. To perform this procedure, a venous stripper is used, and as a reminder this instrument:
• is either inserted into the lumen of the vein—this is referred to as an endoluminal stripper,
• or is placed around the vein—this is referred to as an external stripper.
The advantage of the stripper is that it enables removal of the vein over an extensive length by means of small incisions made at the end of the vein and through which the vein is externalized and removed.
In the early 20th century, three American surgeons codified the technique for stripping of the great saphenous vein (GSV). In 1905, W.L Keller described stripping by invagination (Figure 9) which was revived in 1963 by Van der Stricht under the name of wire invagination (Figure 10). In 1906, C.H. Mayo reported his technique of external stripping (Figure 11). In 1903, W. Babcock popularized endoluminal stripping by using a rigid stripper which remained in favor for several decades.
It would be too time-consuming to describe all the procedures which have marked the history of the stripping technique from the time of the flexible endoluminal stripper recommended by Myers in 1947 to pin-stripping developed by A. Oesch in 1993 (Figure 12). A recently developed stripper even makes it possible to avoid having to make a lower extremity cutaneous incision.
In 1989, R. Milleret described “cryo-stripping” whose principle involves the use of a cryoprobe whose end is chilled to – 60-90°C with nitrous oxide. This probe is inserted into the lumen of the vein and the application of cold “glued” the vein to the catheter which was removed with the cryo-stripper (Figure 13).
Stripping was possibly supplemented by serial phlebectomy and ligation of the incompetent perforator veins to eliminate tributaries presenting reflux. Other teams preferred treating these abnormal tributaries and perforator veins with additional post-operative sclerotherapy.
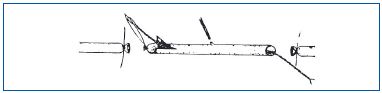
Figure 9. Venous stripping by invagination, Keller (1905). The part of the vein resected between the 2 ligations is invaginated as the finger of a glove into the lumen of the vein from its upper end after attachment to a steel wire pulled through the lower orifice.
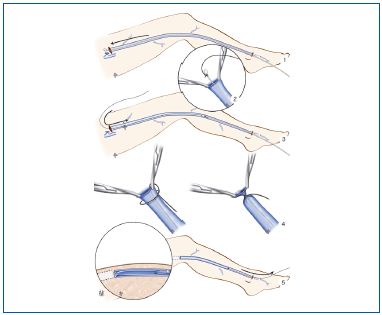
Figure 10. Venous stripping by invagination according to Van der Stricht’s procedure (1963).
Caption: 1. The vein is catheterized with a stripper from the distal incision to the groin.
2. A sturdy wire is attached to the stripper.
3. The stripper is pulled through the vein from groin to ankle, the wire has taken its place.
4. This wire is secured to the great saphenous vein in the groin.
5. Pulling on the distal end of the wire produces stripping of the vein by invagination.
Principes. Techniques. Résultats.
EMC (Elsevier Masson SAS, Paris), Techniques chirurgicales – Chirurgie vasculaire, 43-161-B, 2007.
In 1956, a Swiss dermatologist in Neuchâtel, Dr Robert Muller, gave a boost to phlebectomy by serial incisions under the term ambulatory phlebectomy. He performed this technique as an office procedure under local anesthesia and patients were immediately able to resume walking. He treated all superficial varicose veins with this method. The French and Swiss Societies of Phlebology were somewhat skeptical of this method but, since then, many dermatologists, phlebologists and a certain number of vascular surgeons have taken up this procedure and advocate its use, albeit often limiting its indications to certain types of varicose veins.
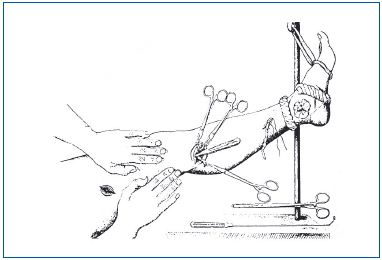
Figure 11. External stripping, Mayo (1906). The external stripper in the right lower part of the original figure contained a ring at its end. This ring was placed around the vein like a thread in the eye of a needle while the previously sectioned vein was placed under tension by pulling on forceps and the tributary veins were successively torn away at the point of emptying into the saphenous trunk by pushing the external stripper from the skin incision below the knee up to that of the thigh. Thus, removal of the vein was achieved closer and closer to the saphenous trunk.
Note elevation of the limb to minimize bleeding: the amount of blood in a vein is reduced by this position.
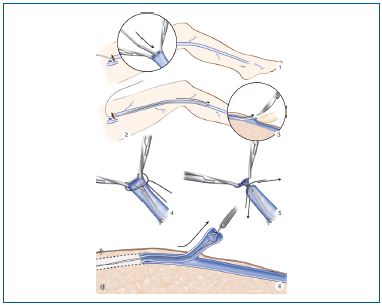
Figure 12. Pin-stripping (Oesch 1963).
Caption:1. The distal end of the pin-stripper is inserted into the venous lumen in the groin.
2,3. The pin-stripper is externalized at the lower end of the vein to be treated after making a minimal skin incision and perforation of the vein.
4,5. The wire secured to the eye hole of the pin-stripper is inserted into the venous lumen by pulling the stripper, and is then secured to the vein.
6. The stripper and the everted vein are removed through the distal incision.
Principes. Techniques. Résultats.
EMC (Elsevier Masson SAS, Paris), Techniques chirurgicales – Chirurgie vasculaire, 43-161-B, 2007.
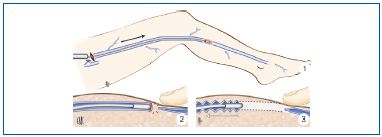
Figure 13. Cryo-stripping (Milleret 1989).
Caption: 1. The cryo-stripping catheter is lowered to the lower limit of the vein to be treated.
2. After freezing, the vein is ruptured by pulling the catheter.
3. The catheter is pulled from the incision in the groin while maintaining freezing. The frozen vein is secured to the catheter. The cryo-stripper is removed through the incision in the groin. The great saphenous vein has remained attached to the catheter by freezing.
Principes. Techniques. Résultats.
EMC (Elsevier Masson SAS, Paris), Techniques chirurgicales – Chirurgie vasculaire, 43-161-B, 2007.
Thermal and chemical ablation
These methods differ from the previous techniques by:
– the absence of ligation of the saphenous vein junction, which eliminates the incision in the groin for the GSV or in the popliteal fossa for the small saphenous vein (SSV).
– the manner of removing the saphenous veins and their incompetent tributaries. Instead of performing excision of these veins, they are destroyed in situ.
English-speaking doctors justifiably use the word “ablation” in this definition, adding the name of the procedure used, for example thermal ablation or chemical ablation. In fact, in science, the word ablation means progressive destruction of a material (a vein, in this case) by a physical agent. Therefore, thermal ablation or chemical ablation eliminates reflux into the treated vein after its destruction and fibrous transformation is obtained. This type of ablation differs from surgical ablation, which removes the organ treated but produces the same result in pathophysiological terms.
It should be noted that these procedures are usually performed by venipuncture of the venous lumen identified perioperatively by ultrasound methods of investigation commonly referred to as Doppler examination, named after the Austrian physicist and mathematician Johann Christian Doppler who in 1842 demonstrated the shift in the frequency of an acoustic or electromagnetic wave between the measurement at emission and measurement at reception when the distance between the transmitter and the receiver vary over time. In fact, the Doppler ultrasound used in phlebology couples an ultrasound device with a Doppler transducer.
As a brief reminder, ultrasound was first used during the Second World War to detect underwater submarines. In 1960, two Japanese scientists, S. Samotura and Z. Kaneko, were the first to apply ultrasound to investigate blood vessels, because blood contains formed elements, the blood cells, which are transported in the circulation in blood vessels, just as submarines travel underwater in the ocean.
Thermal ablation, laser ablation, radiofrequency ablation and steam ablation
These methods have in common the fact that they use a catheter or a fiber which is inserted into the lumen of the vein. The tip of this catheter is heated to a high temperature and applied to the inner wall of the vein, the intima, and the heat is transmitted to the entire wall of the vein. This high temperature destroys the lumen by progressive retraction of the tissues of the wall.
Laser ablation
A laser generator emits monochromatic light which is transmitted to the tip of the fiber. This light energy is converted into heat energy. Without going into technical details, diode and YAG laser fibers are used, whose wavelength and type vary. A laser shot can be performed continuously or discontinuously (Figures 14 a, 14 b, 14 c).
Radiofrequency ablation
This uses the heat properties of an electrical current produced by a generator which is delivered at the tip of a catheter. A certain number of physical parameters can be measured continuously and precisely on the energy delivered by the catheter (Figure 15).
Thermal ablation by high-temperature steam.
Initiated by the Frenchman R. Milleret in 2008, this is based on injection of pulsed steam into the lumen of the vein to be treated, using an electrically heated catheter. The steam condenses at the end of the catheter, transmitting heat to the wall of the vein.
Chemical ablation
This is commonly called sclerotherapy and, like in the thermal ablation methods the use of Doppler ultrasound during the procedure provides safety and accuracy.
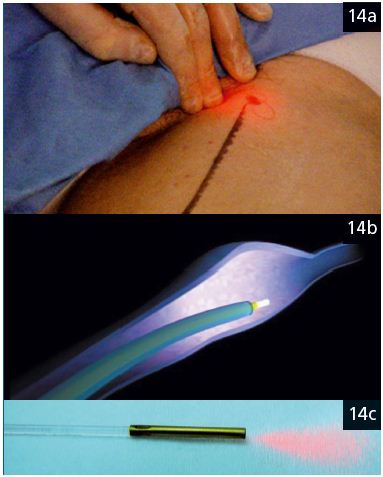
Figure 14 a. Laser ablation method.
The end of the laser catheter can be readily identified under the skin as it advances in the venous lumen.
Figure 14 b. Diagram. The laser catheter in the venous lumen is progressively removed downwards.
Figure 14 c. Protected frontal emission laser fiber. We see the laser light in the axis of the fiber whose end is capped on the side.
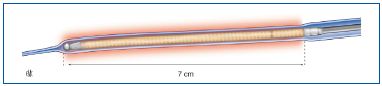
Figure 15. Radiofrequency ablation.
Closure FAST™ Catheter. The circular heating element of the catheter measures 7 cm in length which makes it possible to treat an equivalent length of vein in a few seconds.
But the novel item in sclerotherapy is the use of a sclerosing product as a foam (gas bubbles + sclerosing liquid) instead of the liquid form. This foam must be prepared just before it is to be used because it is unstable (Figure 16). Venipuncture and dissemination of the foam are done using ultrasound guidance (Figure 17).
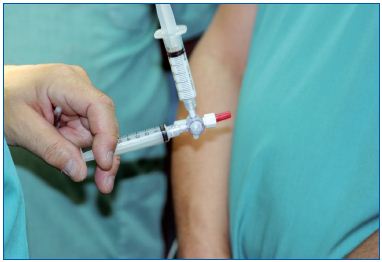
Figure 16. Preparation of foam for sclerosing injection. Twosyringe method according to Tessari’s technique.
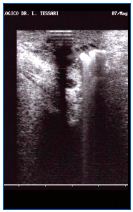
Figure 17. Doppler ultrasound during injection of sclerosing foam. The needle and the foam can readily be identified.
Although use of foam sclerotherapy can be identified as early as 1930, it did not really develop until the last fifteen years or so and the contribution to the promotion of this method by the following people should be mentioned (in alphabetical order): J. Cabrera, A. Frullini, C. Hamel- Desnos, G. Mingo, A. Monfreux, M. Schadeck, L. Tessari, F. Vin. The advantages of this technique have now been well identified and the protocol it uses is well defined.
These are open surgical procedures which use different methods but leave the saphenous trunk in place. Some of them have been abandoned, such as isolated resection over a few centimeters of the ending of the GSV or of the SSV, in which ligation of the GSV was supplemented by ligation of the perforator veins. This procedure was called crossectomy* and was proposed and performed in the 1980s by a team in Sweden.
Currently, 3 procedures with preservation of the saphenous trunk are performed (Figure 18). The rationale for these techniques is based on 2 points: the first is the potential utility of preserving the saphenous trunks which are the best graft material for the replacement of diseased arteries. The second point is that the saphenous trunks promote the drainage of venous blood in the superficial tissues of the lower limb, even if in some case they are the site of partial reflux due to incompetent venous valves.
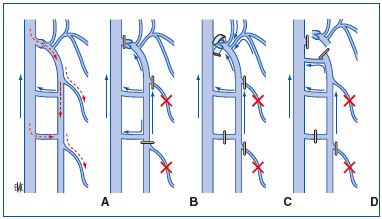
Figure 18. Varicose vein surgery with preservation of the saphenous trunk.
A. Diagram of an incompetent saphenous vein. On the left: deep vein axis. On the right: axis of the saphenous vein and its tributaries. Between the 2 systems: the perforating veins. The blue or white arrows indicate the normal direction of blood flow, the red arrows show reflux.
B. SALVA method. Diagram. The incompetent saphenous trunk is left in place. Only the incompetent tributaries are treated by phlebectomy.
C. CHIVA procedure. Diagram. The incompetent saphenofemoral junction is tied off, the incompetent tributaries are treated by phlebectomy and the saphenous trunk is tied off below re-entry of the perforating vein which returns blood to the deep venous trunk.
D. Diagram The incompetent saphenous vein is left in place. A sleeve is placed on the incompetent saphenofemoral junction, reduction of diameter of the vein restores the anti-reflux function of the terminal valve of the saphenous vein. The incompetent perforating veins are tied off and the incompetent tributaries are treated by phlebectomy.
Principes. Techniques. Résultats.
EMC (Elsevier Masson SAS, Paris), Techniques chirurgicales – Chirurgie vasculaire, 43-161-B, 2007.
A B C D
* Crossectomy (extended saphenofemoral or saphenopopliteal junction ligation).
The origin of this term, a procedure widely used in Germany, Spain, and France, is related to the morphology of the terminal part of the saphenous veins which is curved like the curved part of a bishop’s miter.
These 3 procedures differ in terms of both their technical execution and their hemodynamic objective, keeping in mind that they only require very small cutaneous incisions but call for more specific preoperative Doppler ultrasound examination than the other surgical techniques.
Phlebectomy of tributary veins
For over a hundred years it was considered that progression of varicose vein disease occurred “from the upper area downwards”, as underlined above. But the systematic use of Doppler ultrasound and then of color duplex scanning in assessment of varicose veins called this notion into question:
– Venous reflux can be segmented, that is, highly localized to whatever venous segment;
– Chronologically, reflux does not necessarily develop from the root of the limb toward its distal extremity. In other words, saphenous reflux does not always begin at the saphenous vein junction into the deep veins. It can start in the tributary veins of the saphenous trunks.
This origin of reflux was demonstrated by N. Labropoulos (USA) in 1997 and has been confirmed by many studies.
Lastly, the degree of reflux and probably its progressive extension are promoted by the capacity of the reservoir in which this reflux can be evacuated. Compression of an incompetent tributary vein at its mouth, into which an incompetent saphenous trunk termination empties, partially or totally eliminates reflux in it (Figure 19). This process was mentioned in 1993 by French phlebologists.
In 1995, based on these findings P. Pittaluga (Nice, France) proposed phlebectomy of tributary veins to restore valvular competence of the GSV trunk, using the acronym SAVLA (Selective Ablation of Varicose Veins under Local Anesthesia) (Figure 18b).
The CHIVA procedure (hemodynamic preservation in venous insufficiency in ambulatory practice)
Proposed in 1988 by Franceschi (France), CHIVA is designed to create new hemodynamic conditions by dividing the pressure column in the varicose veins by disconnecting some venous anastomoses and by redirecting the reflux from the diseased superficial veins into the deep venous system (Figure 18c).
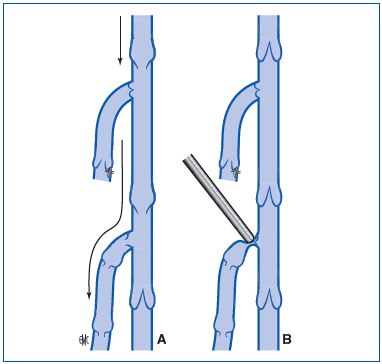
Figure 19. Decrease in capacity of the reservoir to reduce or eliminate the reflux.
A. The reflux in the primary venous trunk is drained into a tributary vein whose valves are incompetent. This “drain effect” increases the degree of reflux into the primary trunk.
B. Compression of the tributary at its point of emptying into the primary venous trunk eliminates the reflux into it.
EMC (Elsevier Masson SAS, Paris), Techniques chirurgicales – Chirurgie vasculaire, 43-161-A, 2007.
Valvular reconstruction
The terminal valves of the GSV can be treated by such reconstruction. The principle consists in restoring valvular competence by using different procedures to eliminate reflux through these valves: valvular repair (L. Corcos, Italy 1997), and exo-stent repair of the junction to reduce the diameter of the vein (S. Camilli, Italy 2002, J.R. Lane, Australia 2002) (Figure 18d). It should be noted that the therapeutic principle is based on the so-called “descending” theory of varicose vein disease as in traditional open surgery.
Perforating vein surgery
Although incompetent perforator veins are not peculiar to chronic venous disease, it is when they are associated with varicose veins in patients presenting with venous ulcer that they are treated surgically. In fact, when they are incompetent, they are responsible for reflux from the deep venous system towards the superficial venous system, which produces a constant increase in venous pressure. The latter is consistently identified in venous leg ulcers. R. Linton (USA, 1939) and then F. Cockett (United Kingdom, 1955) successively identified the role played by perforating veins in the occurrence of venous ulcer. They specified ligation of these veins by open surgery. These techniques had the disadvantage of producing delayed healing of cutaneous incisions when the skin is fragile. To compensate for this complication, Hauer (Germany, 1985) proposed endoscopic surgery on the perforating veins. This procedure gradually benefited from miniaturization of the instruments used (Figures 20 a, b, c).
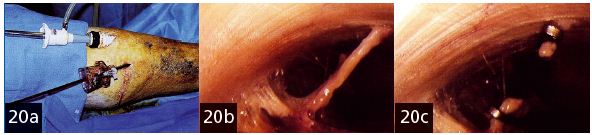
Figure 20a. Subfascial endoscopic perforator surgery. Same surgical view.
Figure 20b. The perforating vein as the surgeon sees it on the video screen.
Figure 20c. Idem, after sectioning between the 2 clips.

