NEW TECHNIQUES – Part 1
Classical operations for varicose veins (VV) are performed less and less. The increasing use of foam sclerotherapy and various endovenous closure devices (endovenous laser therapy (EVLT), VNUS® radiofrequency closure) rather than classical surgical management is becoming evident. These less invasive therapies allow treatment of older people who in the past would have been treated only by compression. Prof J. J. Bergan (USA) pointed out that with these techniques the classical surgical approach to the saphenofemoral junction in VV disease is only necessary in cases with venous aneurysms exceeding 2 cm in diameter at the level of the preterminal valve in the junction.
VEIN DISEASE
Moderators: L. GRONDIN (Canada), N. SADICK (USA)
1320 nm endovenous laser treatment of the greater
saphenous vein (GSV)
M. P. GOLDMAN (USA)
Most papers on endovenous laser treatment (EVLT) describe the use of laser frequency of 810 nm or 980 nm. The chromophore of these frequencies is hemoglobin. The heat of the laser tip is approximately 1000° C, causing the blood to boil. This leads to pain and bruising, and may sometimes result in perforation of the vein wall. The author of this paper describes his experience with a laser of 1320 nm on 50 patients with varicosities of the GSV. The higher frequency of the laser has water as its target structure therefore acting directly on the vein wall. Bruising and pain were significantly decreased compared with the other lasers used in that indication.
Radiofrequency ablation of refluxing superficial
and perforating veins using VNUS closure and transluminal
occlusion of perforator veins
M. WHITELY (UK)
The author reported extensive experience on RF closure procedures in 1022 legs with varicose veins.
In contrast to other centers only treating GSV and SSV varicosities, veins treated were:
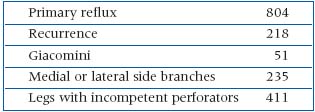
Alfentanyl preventing venospasm was used in order to ascertain complete closure by the RF treatment. Local anesthesia can produce a venospasm mimicking successful therapy. No local anesthetics were used, as general anesthesia was necessary due to the apnea induced by the alfentanyl.
The excellent results seem to warrant this method.
The rates of complete occlusion with resulting atrophy was as follows:
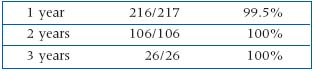
Chairpersons: T. PROEBSTLE (Germany), S. E. ZIMMET (USA)
Speakers: S. M. DOSICK (USA), R.F. MERCHANT (USA), K. L. TODD,
III (USA), T. PROEBSTLE (Germany), R. MILLERET (France),
R. J. MIN (USA), A. TZILINIS (USA)
The session was devoted to various aspects of radiofrequency ablation (RFA) and endovenous laser treatment (EVLT).
S. M. Dosick compared RFA in treatment patients older than 70 years with that in patients younger than 70 years. He did not find significant differences in the postoperative and rehabilitation period in this group (35 patients, 41 limbs) in comparison with patients <70 years (386 patients, 449 limbs). Forty percent of patients of the group >70 years had active/nonactive ulcers. All ulcers were healed by 3 months after operation. The author concluded that RFA can be a safe method for treatment of older patients with intercurrent pathology.
R. F. Merchant successfully performed RFA for treatment of 10 patients with insufficiency of the short saphenous vein (SSV). Successful, complete closure of the SSV was achieved in 10/10 (100%). No complications occurred. The author concluded that RFA can be use for safe treatment of SSV reflux. Different types of diode lasers (810 nm, 940 nm, 980 nm) have been used for EVLT.
K. L. Todd presented a series of patients with 386 greater saphenous veins (GSV) treated with EVLT. All patients were evaluated with duplex ultrasound at intervals varying from 3 to 12 months; 377 GSV had no reflux postoperatively. The author concluded that EVLT is an effective method for long-term venous ablation.
R. J. Min presented the follow-up results of EVLT in 610 patients (701 limbs). There were GSV (566 limbs), SSV (65 limbs) and anterior-lateral tributaries (70 limbs). The 2-year follow-up demonstrated a recurrence rate of less 7%.
T. Proebstle presented the detailed description of EVLT technique and mechanism of the GSV obliteration. The author had experience of EVLT in 85 patients (104 GSV) with CVI clinical stage C 2 to 6. He demonstrated that endovenous laser produces small steam bubbles which mediated heat injury to the endothelium with secondary thrombotic occlusion. The author discussed how different endovenous methods influence vessel shrinking and thrombus formation (Table I).

R. Milleret compared the results of various methods of the endovenous treatment of incompetent GSV (RFA, EVLT and catheter-delivered foam sclerotherapy (Table II).
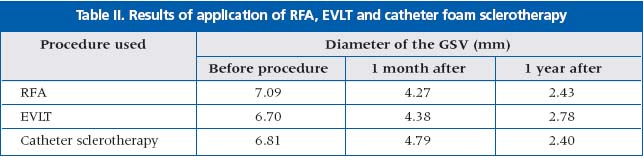
Complete disappearance of the vein lumen was achieved in 8/25 cases with RFA and 4/25 cases with EVLT.
A. Tzilinis used a Quality of Life (QOL) questionnaire for an estimation of the RFA results. This specific questionnaire was developed by Launois (1996) and has been successfully validated in the well known RELIEF study. A. Tzilinis concluded that RFA of the incompetent GSV significantly improves patient’s QOL. The average preoperative score was 49+15, decreasing postoperatively to 29+10, for a 41% improvement (P<0.001).
Chairpersons: J. J. Bergan (USA), R. A. Weiss (USA)
Review of the use of foam
A. FRULLINI (Italy)
Sclerosing foams (SF) are mixtures of gas and liquid solution with surfactant properties, affording full control of drug concentration inside the vein and contact time with the endothelium. Cabrera proposed the use of a microfoam of sodium tetradecyl sulfate and polidocanol for sclerotherapy in 1993. Many authors subsequently reported different methods for foam production. Sclerosing foam is characterized in part by the following parameters:
• type and concentration of sclerosant
• type of gas, ratio of liquid to gas
• additional nonactive substances
• the method of preparation
• the time after processing
• bubble size distribution.
Now, several pharmaceutical companies have become interested in foam. For example, a British company is developing a fully characterized microfoam (Varisolve™ – Provensis, UK) made to approved pharmaceutical standards.
The science of microfoam
T. HARMAN (UK)
Amicrofoam has a number of unique physical properties. Bubble size, fluid-to-gas ratio, and foam breakdown rate are all highly important. New measurement techniques were developed to define the essential differences between microfoams, foams, and froths, depending on the diameter of bubbles:
• froth >500 mm
• foam >300-500 μ
• microfoam <250 μ
Microfoams are characterized by:
• density
• stability
• bubble size distribution.
Density is controlled by the ratio of fluid to gas. Stability is dependent on viscosity, dissolved gas, temperature, and bubble homogeneity. The most important criterion for microfoam stability is half separation time (HST). HST is the time taken for half the liquid component of the microfoam to separate from the gas. Bubble size distribution measurement is complex and must also be performed quickly. Further examination of properties of microfoam intended for medical purposes is necessary.
Safety of intravenous foamed sclerosants
D. WRIGHT (UK)
Superficial thigh veins of dogs were injected with 1% polidocanol microfoam, 5 mL/sec. Pulmonary artery pressure (PAP), mean systemic arterial pressure (MAP), EKG, transesophageal echo-ultrasound, O2 saturation, and tidal CO2 were continuously recorded. Cardiac output and pulmonary and peripheral resistance were measured. Three dosage models were investigated (single, multiple with fixed interval, and multiple with variable interval). A significant, rapid, and dose-dependent rise in PAP and fall in MAP followed injections >10 mL. Thus, sclerosant microfoam injected in dogs caused significant pulmonary hypertension and depressed cardiopulmonary function.
European randomized controlled trial of Varisolve® PD
microfoam compared with alternative therapy in management
of moderate-to-severe varicose veins: preliminary results
D. WRIGHT (UK)
Seven countries (France, Belgium, Sweden, Germany, Netherland, Italy, UK) took part in the prospective study of the clinical application Varisolve® foam. Aims of this study were:
• to demonstrate the safety and efficacy of Varisolve® in the treatment of moderate-tosevere varicose veins
• to compare the safety and efficacy of Varisolve® using 1% polidocanol with best alternative conventional treatment for varicose veins (surgery or sclerotherapy).
Varisolve® microfoam was injected under ultrasound control into incompetent trunk veins. Posttreatment follow-up evaluation included duplex ultrasound, photography, and Launois’s (1996) Quality of Life questionnaires. The end point was the elimination of reflux and occlusion of the affected trunk vein. For the purposes of the study 658 patients were recruited. They were divided into three groups:
• 654 patients treated – 435 Varisolve® -125 sclerotherapy – 94 surgery
• Age mean 50.0 (SD 12.2) range 19-75
• Sex 68.2 female, surgery cohort 63%, sclerotherapy 71%
• Great sapherous vein (GSV), 83.3% mean diameter 7.44 mm
• Short sapherous vein (SSV), 19.5% mean diameter 6.55 mm
• Recurrent varicose veins, 13.6%
There were 14 related adverse events (Table I).
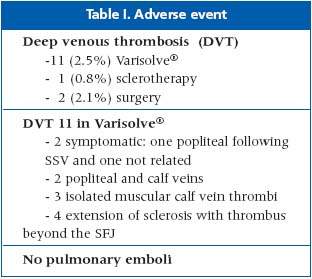
The elimination of reflux was achieved during 3 months’ follow-up in all treatment groups. Thus, Varisolve® microfoam has similar short-term efficacy to flush ligation and stripping. Sclerotherapy, while least invasive, was also least effective.
French experience with Varisolve® PD microfoam in the
management of moderate to severe varicose veins
J. P. GOBIN (France)
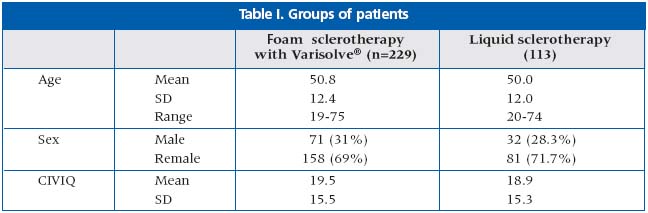
The study included 342 patients with greater (GSV) and/or short saphenous vein (SSV) incompetence, with moderate-to-severe varicosities. All patients were divided into two groups according to method of sclerotherapy (Table I).
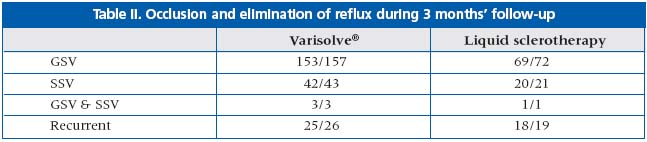
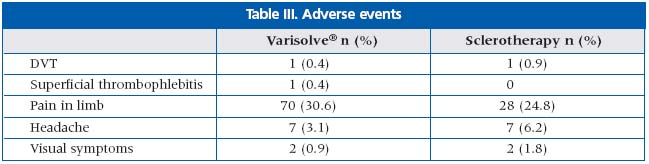
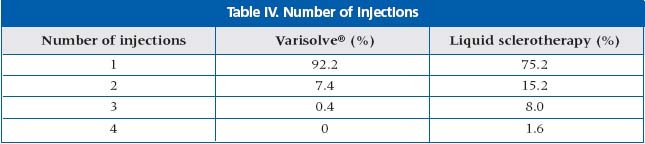
The results of application of Varisolve® sclerotherapy were compared with liquid sclerotherapy (Tables II, III, and IV). It was the preliminary conclusion that Varisolve ® sclerotherapy provides high efficiency, little discomfort, and few complications.
Ultrasound-guided injection of polidocanol microfoam in the
management of venous leg ulcers
J. CABRERA GARRIDO, A. BECERRA, M. COBO, C. GARRIDO, M. CABRERA Jr (Spain)
One hundred and seventy-one patients (180 limbs) with venous ulceration were treated. The mean age of patients was 58.5 years, and 8.33% of them were older than 75 years. The mean duration of the ulcers was 5.8 years. The reasons for ulceration were greater saphenous incompetence (147 limbs), deep venous reflux (55 limbs), and perforator vein incompetence (98 limbs). Ultrasound-guided injection of polidocanol microfoam was performed in all cases for reducing venous hypertension. One hundred and sixty-three (90.6%) ulcers were healed over 3.7 years’ follow-up (mean rate 2.7 months) without serious complications. There were 28 recurrences of ulcers in this group, which needed additional treatment.
Testing foam made on-site for sclerosing varicose veins
S. SADOUN (France)
There are two tests for estimation of quality of the foam in vitro.
Test A: On a flat piece of glass, a drop of foam is deposited to calculate the time the foam return to a liquid form.
Test B: A drop of foam is deposited on an inclined (15o) piece of glass: the time it takes to reach the bottom determines the foam’s adhesiveness to the surface.
It is obvious that stability and adhesiveness lead to better results.
Foam closure of the long saphenous vein:
preliminary report
R. GONZALEZ ZEH (Chile)
Twenty-eight patients (33 limbs) with long saphenous vein (LSV) incompetence were treated. Polidocanol 3% foam (10 cc per session) was injected into the LSV. Ultrasound duplex control was obligatory. Class I compression was used for 3 months. There were no serious complications over 24 months’ follow-up. Distal transient parasthesias were found in 6% of limbs. Eighty-five percent of LSVs were closed during 24 months’ follow-up.
Endoluminal therapy with echo-guided sclerosant foam:
current situation after 30 years of experience
A. L. CABRERA GARRIDO, B. CABRERA NYST (Spain)
Therapy with sclerosant foam of soluble gases and detergents offers four important advantages:
• Lower dose of sclerosant
• Increase tolerability to extravasation
• Accurate echographic control of application area
• Sclerosant agent and its action stay in situ.
There are more important principles of the effective and safe application of the foam-form sclerotherapy:
• An accurate and complete anatomohemodynamic venous map
• Formulations in accordance with objectives of sclerosant foaming agent
• Stable and consistent foam obtainable using special technical procedure
• Complete intervention on first session
• Ultrasound evolutionary short-term and medium-term monitoring for early detection and secondary treatment recurrences.
• Detailed list of essential technical instruments
Microfoam ultrasound-guided sclerotherapy for varicose
veins in a subgroup with diameter at the junction of >10 mm
compared with a subgroup <10 mm
J. M. BARRETT, M. COLDMAN, B. ALLEN, A. OCKELFORD, K. JACOBSEN (New Zealand)
Sixteen legs with long saphenous veins (LSV) with a diameter at the junction of >10 mm (average diameter 12 mm) were compared with 97 LSVs with a diameter at the junction of <10 mm. Ultrasound-guided sclerotherapy (UGS) was performed in all cases. Patients were asked to complete a “quality of life” questionnaire by Launois (1996). Post-sclerotherapy examination included visual and Duplex ultrasound assessment.
Results of investigations are presented in Table I.
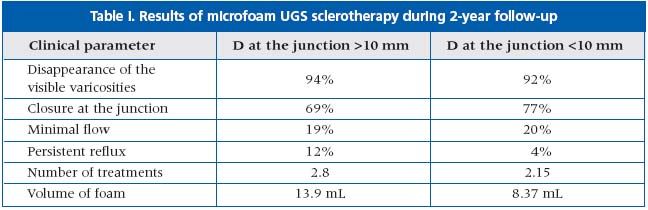
Patient satisfaction parameters were very similar for both groups. Thus, foam UGS sclerotherapy is equally effective for treatment of varicoses in LSV with diameter at the junction >10 mm.
Results of a European consensus meeting on the use of
foam in sclerotherapy of varicose veins
F. X. BREU (USA), S. GUGGENBICHLER, E. RABE (Germany)
A European Consensus Meeting on the use of extemporary foams in sclerotherapy of varicose veins took place in Tegernsee, Bavaria, Germany in April 2003. The purpose of this meeting was to reach a consensus and come up with practical suggestions on foam sclerotherapy, including diagnosis, indications and contraindications, equipment, therapeutic strategies, application of sclerosing foam, efficacy, adverse events and complications, post-sclerotherapy treatment, etc. More than 20 experts from different European countries actively discussed the subject. All participants agreed that the use of sclerosing foam is an appropriate procedure in the therapy of varicose veins. Sclerosing foam is a powerful tool in expert hands and in general more effective than the liquid form of sclerosants. It is necessary to have good skills in conventional liquid sclerotherapy before starting with foam sclerotherapy.
Chairpersons: J. J. GUEX, (France), R. A. WEISS (USA)
Aethoxysclerol foam obliteration of insufficient
perforating veins in patients suffering from leg ulcers:
a clinical recommendation
Z. RYBAK (Poland)
To assess the influence of elimination of venous reflux on the healing of leg ulcers, 40 patients were enrolled and divided into two groups randomized according to their age, sex, and the history of the disease, and treated with conservative treatment for one group or by foam sclerotherapy for the other group.
The authors concluded that the obliteration of insufficient leg perforators increased the rate of healing in ulcers. Results are shown in Table I.

Echo-sclerotherapy of the greater saphenous vein by direct
puncture using sclerosing foam
C. HAMEL-DESNOS, J. J. GUEX, P. DESNOS, et al (France)
The authors compared the efficacy of polidocanol foam versus liquid for echo-sclerotherapy of the greater saphenous vein by direct puncture. They tried to assess the reproducible evidence of the efficacy and the safety of this method.
After 2 years’ follow-up the authors stated that in order to avoid disappointment and accidents this technique requires knowledge of foam preparation, manipulation, and injection, as well as experience in conventional liquid sclerotherapy and venous echo-Doppler.
Treatment of venous aneurysm with foam sclerotherapy
G. BELCARO, M. R. CESARONE (Italy), K. MYERS (Australia)
The authors reported the example of a 65-year old woman who complained of the existence of a lump located at the third, internal part of the left femoral fold. The lump was painless and easily obliterated by compression. Color duplex scanning showed a large cavity (4x4x6 cm) with venous flow visible. The authors performed two obliteration sessions (0 and 2 weeks) with the guidance of ultrasound, by means of foaming agent. To avoid passage of sclerosing foam into the femoral vein, compression of the femoral vein was used. After 4 weeks the authors obtained a complete occlusion of the aneurysm which was confirmed 12 weeks later, and they hope that this method, never described before, will prove to be a good solution in the treatment of venous aneurysms.
Treatment of severe CVI with sclerosant foam
J. J. BERGAN, L. V. MEKENAS (USA)
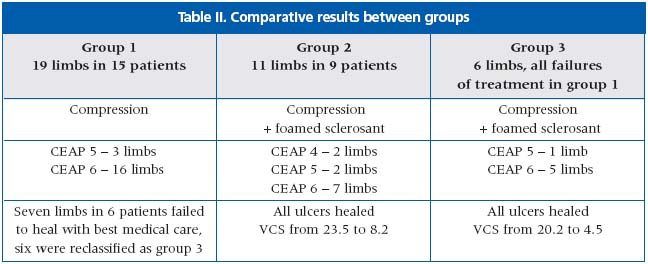
To assess the usefulness of foam sclerosant in treatment of CVI classes 4, 5 and 6, 30 limbs in 24 patients were enrolled in the study. Venous clinical severity (VCS) and the healing of the lesion were considered as end points.
The data are presented in Table II.
The authors consider the advantage of sclerotherapy with foamed sclerosant over compression therapy of severe CVI. Used early it can shorten treatment time.
Microfoam ultrasound- guided sclerotherapy for varicose
veins in a subgroup with diameter at the junction >10 mm
compared with a subgroup < 10 mm
J. M. BARRETT, M. P. GOLDMAN, B. ALLEN, et al (New Zealand)
The authors analyze the efficacy of ultrasoundguided sclerotherapy for varicose veins. By means of an improved foam-making technique, they could reach 90% efficacy after the first injection. The diameter at the junction does not influence the final treatment results.
Color duplex imaging and intraoperative assessment of
terminal valve competence at the saphenofemoral junction
A. CAVEZZI, C. TARABINI, M. G. BARBONI, et al (Italy)
The results of a multicenter prospective comparative study (18 patients with varicose veins- C2-C5) were collected and analyzed. Preoperative data regarding greater saphenous vein incompetence without reflux at the terminal valve (TV) of the saphenofemoral junction (SFJ) were compared with intraoperative assessment of competence of the TV at SFJ. To assess possible blood reflux from deep veins through the SFJ the GSV 2 to 4 cm below the SFJ was cut off by the authors without division of tributaries, and then the Valsalva maneuver and manual compression of iliac fossa were performed. Four out of 18 patients had slight reflux in the GSV stump. When the lower tributaries were disconnected, three out of those 4 still had reflux, and no reflux was observed when the upper tributaries were disconnected. These interesting findings can lead us to the conclusion that in the presence of competent TV, retrograde flow in GSV can derive from saphenous tributaries.
Moderators: M. P. GOLDMAN (USA), A. FRULLINI (Italy)
A randomized clinical trial comparing the effects of foam vs
liquid formulas for sclerotherapy of primary varicose veins
Perfluoropropane-filled albumin microspheres-sodium
tetradecyl sulfate vs air-filled sodium tetradecyl sulfate for
foam sclerotherapy of great saphenous vein incompetence
P. RAYMOND MARTIMBEAU (USA)
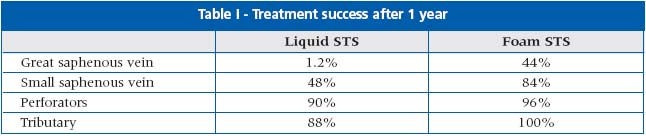
The author presented two studies with similar methodology in similar groups of patients. The first study compared liquid vs foam sodium tretradecyl sulfate (STS) in patients with varicose veins. The efficacy and the safety of the foam preparation were greater compared with the patients treated with the liquid formula. (Table I)
In the second study a group treated with the foam preparation of STS 1% was compared with another group treated by perfluoropropane-filled albumin microspheres prior to injection of the STS foam in order to obtain a vein devoid of blood. The perfluoropropane-filled albumin microspheres – sodium tretradecyl sulfate preparation worked better concerning effectiveness and side effects.
Foam echosclerotherapy of incompetent saphenous veins
L. GRONDIN (Canada)
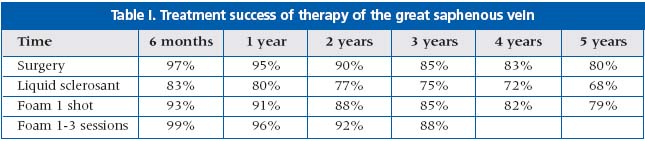
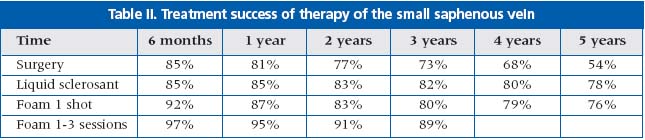
The author described his work with a foam preparation on a basis of CO2 enabling him to use larger quantities (up to 25 cm3) of the therapeutic preparation. CO2 based foams have freater safety when compared with air-based foam, as CO2 is 20 times more soluble than air. It is therefore less likely to cause air embolism-related symptoms such as chest pain and transient ischemic attacks. These have been described as rare, but there are major side effects with air-based preparations, especially when larger volumes are given. Foam preparations have been found to be superior to liquid sclerotherapy, especially in patients with recurrent varicose veins. The results of foam sclerotherapy were comparable to those of surgery at the 5-year follow up. (Tables I, II)
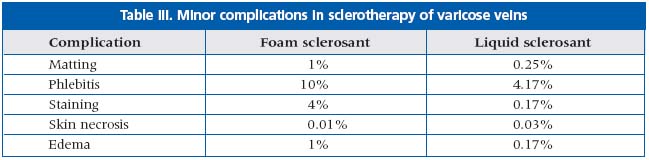
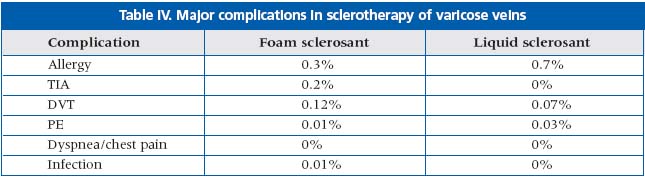
Side effects were more frequent and more pronounced in the foam sclerotherapy treated population. Thromboprophylaxis was suggested in risk patients. (Tables III and IV)
PHLEBOLOGY NURSING
Chairpersons: A. FRONEK (USA) , M. GEORGIEV (Italy)
Leg Clubs:
a patient-centered approach to leg ulcer management
E. T. LINDSAY (UK)
The main determinant for the development of leg ulceration in chronic venous disease is ambulatory venous hypertension, which acts through damage of the microcirculation. To improve the treatment of venous leg ulcers the authors have created “Leg Clubs” which are a new type of clinic where management is intensified. Leg Clubs offer a unique partnership between patients, nurses, and the local community, and are characterized by four features:
1. Based on the community, nonmedical environment
2. Collective treatment
3. No appointment required for the operation
4. Patients have a fully integrated “well leg” regime.
The authors concluded that only such an attitude to leg ulcer treatment can enhance patient compliance, healing rates, and patients’ quality of life.
Practical application of ultrasonography in assessing deep
and superficial venous dynamics
S. X. SALLES-CUNHA (USA)
The author described the relationship between prevalence of reflux and diameters in the superficial veins of the lower extremity. They have used them as a guide for prosthetic valve implantation in the deep veins as well as in assessing the results of such treatment. Duration of reflux, maximum reverse velocity, and diameter of deep, superficial, and perforating veins were measured by means of B-mode color flow ultrasonography.
The authors stated:
a) On the basis of the amount of reflux and vein diameter, endovascular prosthetic valves were implanted in the proximal femoral vein.
b) Perforating veins with a diameter larger than 4 mm always result in reflux.
c) Early symptoms are not associated with reflux in the saphenofemoral junction but with segmental reflux.
d) Deep vein diameters vary under conditions of vasoconstriction and vasodilatation.
Vein stripping: is it an obsolete procedure?
S. HIRSCH (USA)
According to published data there is strong evidence to state that saphenous stripping is the best procedure to guarantee a low percentage of recurrences. The most frequent cause of recurrent varicose veins after surgery appears to be the presence of incompetent perforators. The rate of failure is higher if the long saphenous vein is conserved. However, some authors have indicated that although long saphenous vein preservation could lead to recurrences in a small number of cases, at the same time it prevents nerve injuries and scars. By complete exposure of the common femoral vein and identification and ligation of all the tributaries and incompetent perforators, without stripping of the long saphenous vein, a recurrence rate of only 12% can be achieved. Because the closure of the greater saphenous vein, either with radiofrequency, laser, or sclerotherapy has become a more and more acceptable procedure, it appears that in most situations saphenous incompetence can be treated only by closure with low recurrence rate.
A new vein in ultrasonic view
P. ZAMBONI, M. DE PALMA, S. CARANDINA, et al. (Italy)
The authors described a vein belonging to the saphenous compartment of the leg. They operated on 218 patients who suffered from primary varicose veins. To assess the great saphenous vein tributary and the presence of its homodynamic involvement in varicose networks Duplex scanning before the operation was performed. In 7% of patients a tributary in the saphenous compartment of the medial aspect of the upper third of the leg was observed. It runs transversally in the interfascial compartment toward the lateral aspect of the leg for a length ranging 5 to 12 cm. A complete dissection must be done to avoid recurrences.
Compression and compliance
C. L. MORGAN, B. B. BLONDEAU, L. L. TRETBAR (USA)
Two groups of patients over two periods of time (1994-1998 and 1998-2003) were compared regarding the medical benefits of compression therapy. The authors considered: age, sex, physical limitations, economic limitations, quality of life assessment, and miscellaneous complications. Significant improvement in compliance following detailed instruction and education about compression therapy was observed in the period 1998- 2002.
The conclusion was that the more educated the physicians the better treatment the patients received.
Current concepts of chronic venous disease based
on duplex scaning
N. LABROPOULOS (USA)
Duplex ultrasonography seems to be the ”gold standard’’ in the diagnosis of chronic venous diseases (CVD). The main risk factors remain: age, sex, and family history.
Several studies have shown that both reflux in the superficial veins and reflux or obstruction of the deep venous system result in severe venous ulceration. One cannot ignore the role of perforators in the development of signs and symptoms of CVD and ulcerations. Perforator vein incompetence in the ulcerated area was detected in 28% of ulcers, and it was always associated with superficial and/or deep vein incompetence. The distribution and extent of reflux is associated with the severity of the disease but the strength of this association has not been determined because there are other reasons, such as disease duration, rate of progression, and lifestyle that play an important role.
