NEWS IN RESEARCH – Part 4
Chairpersons: J. MAURIELLO (USA)
and E. RABE (Germany)
Microvenous valves in the normal human lower limb and
chronic venous insufficiency (CVI)
A. M. VAN RIJ (New Zealand)
Contrary to previous belief, venous valves are present not only in the macrocirculation but in microcirculation of normal limbs, and in patients with CVI. Using electron scanning microscopy, microvenous valves were observed in veins down to 20 μm in diameter in the superficial venous system. The regional distribution of valves and the size of veins containing valves were not significantly different in the normal and in venous ulcerated limbs. The concentration of the valves was greater in the proximal parts of calf than in distal parts. Differences were observed in the total density of valves for the same compartment in both groups – patients with ulcerated limbs had a greater concentration of valves and vessels than the control group (153.8 versus 15.1 vessels / cm3, P <0.01). The ratio of vein diameter to valve sinus depth in patients with CVI was significantly greater than in normal (0.85 versus 0.61, P <0.001). In the patients with CVI, retrograde flow in microveins was observed similar to that in the macrocirculation. This is now recognized as another factor, leading to pathological skin changes.
Management of recalcitrant venous leg ulcers
J. D. D. VUERSTEAK (Netherlands)
Recalcitrant ulcers still present a great therapeutic problem. The author presented 5 years’ results of healing recalcitrant venous ulcers using a subatmospheric pressure treatment called vacuum assisted closure (VAC). Twenty four patients with venous ulcer were treated. Patients were divided into two groups – treated conventionally and with the VAC method. Compared with conventional wound care techniques a reduction in the total healing time was seen in VAC-treated ulcers of up to 21.6%. The authors of this presentation believe that the VAC technique will become an important treatment within dermatology, not only for chronic and recalcitrant venous leg ulcers but also for arteriosclerotic and combined inoperable venoarterial leg ulcers.
Local endothelial function and leg symptoms in patients after
deep vein thrombosis
D. N. KOLBACH (Netherlands)
In the authors’ opinion, venous hypertension could lead to endothelial dysfunction, which might be expressed in local abnormalities of coagulation and fibrinolysis. They studied 15 patients with ultrasound-documented DVT in stages C-0 to C-4 of the CEAP classification. All subjects underwent ambulatory venous pressure measurements. Blood was collected from the distal part of legs and arms after 10 minutes’ standing. In patients with DVT there was a significant increase in fibrinogen and von Willebrand factor concentrations in samples from the legs. In the authors’ opinion this indicates local endothelial dysfunction, which may lead to disturbances in coagulation.
Venous reflux measurement:
(a) variability of a standardized Valsalva maneuver and
venous reflux measurement
(b) comparision of a standardized Valsalva maneuver and
compression method
C. JEANNERET (Switzerland)
The author made a comparison between standardized Valsalva maneuver and the pneumatic compression method described by van Bemmelen. In this study 110 vein segments of 55 patients (25 M/30 F, median age 50.6 y, 24.7-71.9) with deep venous insufficiency in varicose vein disease were investigated. The standardized Valsalva maneuver (forceful expiration in the tube system, expiratory pressure of 30 mm Hg within 0.05 s held at least a 3 s) and the standardized compression method (80 mm Hg pressure distal to the investigated vein segment, held for 3 s, pressure released within 0.3sec) were performed. The common femoral vein (CFV) and the superficial femoral vein (SFV) were investigated with duplex sonography (ATL HDI 3000). Venous reflux time (RT), peak velocity (PV), and volume flow (VF) were measured with patients standing. The correlation coefficient for the RT, PV, and VF amounted to 0.71, 0.42, and 0.6 in the CFV; and to 0.63, 079, and 0.65 in SFV. No agreement was found 14 times in the CFV (Valsalva method more sensitive P = 0.002) and 7 times in SFV. The author concluded that Valsalva and the compression method correlate best for reflux time and flow volume in the CFV and the SFV, but the Valsalva method is more sensitive in detecting venous reflux in the CFV. In this presentation were shown individual changes for parameters of venous reflux in the same compartments in following days, independent of the method of measurement used.
Is there duplex ultrasound evidence of neovascularization of
the saphenofemoral junction following endovenous catheter
ablation (EVCA) techniques – 3 years later?
N. MORRISON (USA)
Neovascularization has been found to be a major contributor to recurrent lower extremity superficial reflux following crossectomy with or without stripping. An alternative to stripping is endovenous catheter ablation (EVCA) which has been shown to successfully obliterate the great saphenous vein and preserve the superficial epigastric vein. The author hypothesized that EVCA used in conjunction with ultrasound-guided sclerotherapy will not result in neovascularization and may prove to be a more effective choice in the treatment of reflux of the greater saphenous vein. In a group of 25 patients treated with EVCA and sclerotherapy there was not any revascularization observed after 3 years’ follow-up. In conclusion the author suggested that EVCA with ultrasound-guided sclerotherapy may be a good alternative for replacing vein stripping.
Gene expression profiles in varicose veins using cDNA
microarray
S. J. LEE (Korea)
With cDNA microrray technology we can determine the differential mRNA expression profiles of a huge number of genes, between normal and pathologic specimens. Four patients with varicose veins and normal veins were analyzed. Among upregulated genes in the varicose veins, fibronectin, versican, osteonectin, transforming growth factor, gelsolin, and connective tissue growth factor showed more than twofold increased activity. Although these findings give us insight into changes at the molecular level, these are probably secondary rather than primary factors.
AND NEW RESEARCH
Chairpersons: R. J. MIN (USA) &
U. SCHULTZ-EHRENBURG (Germany)
Prognostic value of dynamic venous function tests with
respect to postoperative hemodynamic outcome
M. JUENGER (Germany)
As Professor Juenger points out, it is interesting to know the exact characteristics of venous problems and to predict the results of a specific surgical treatment in our daily practice. He presented a group of 30 patients (CEAP C2-6) who were studied before and after the practice of a crossectomy plus a saphenous vein stripping in order to test whether dynamic venous function tests could predict postoperative outcome. The venous reflux and the refilling time of the leg were measured using five different methods: phlebodynamometry, three types of photoplethysmography, and dynamic strain gauge plethysmography. Preoperatively the surgical procedure was simulated with tourniquets. The authors found a strong linear relationship between the preoperative simulated results and the postoperative situation with phlebodynamometry, strain gauge plethysmography, light reflection rheography, and light reflection plethysmography. These facts led to the conclusion that the improvement achieved with surgery can be predicted preoperatively by any one of the above tests.
Experience with the CEAP classification in a large
epidemiologic study- the Bonn vein study
E. RABE (Germany)
The German Society of Phlebology initiated an epidemiological study to evaluate the prevalence and risk factors of chronic venous diseases in the general population. From October 2000 to March 2002, 3072 members of the general population of the city of Bonn and two rural zones (age 18 to 79 years, 1350 men,1722 women) were selected via simple randomization from population registries. They answered a questionnaire, and were examined by clinical means and duplex ultrasound. The CEAP classification was used, showing a distribution as follows C0 9.6%, C1 59%, C2 14.3%, C4 2.9%, C5 0.6%, and C6 0.1%. Pitting edema (C3) was present in 13.4%. As a conclusion, the use of the CEAP classification in epidemiological studies must be improved.
Obesity and severity of venous insufficiency
A. M. VAN RIJ (New Zealand)
The correlation between obesity and venous disorders is not clear. Theoretically obese people have a higher intrabdominal pressure that may decrease venous return and increase venous reflux. Defining as obese people with a body mass index (BMI) higher than 30, the author performed an evaluation of the venous refilling time and muscular pump function, finding a shorter refilling time and better muscle pump function when compared with general population. By studying a varicose vein population, he found a larger size superficial femoral vein diameter, a higher venous pressure and a higher percentage of venous ulcers in obese people. This was particularly true in women. As a conclusion, he indicated that obesity worsened varicose veins, but more studies are needed to confirm these findings.
Pathophysiologic assessments of primary varicose veins with
duplex scanning
M. SAKATA (Japan)
This Japanese team presented their extensive experience in studying varicose vein population by means of duplex scan. Duplex scanning was used to examine 1606 limbs with primary varicose veins. Seventy-five percent of them (1205 limbs) had reflux at the saphenofemoraljunction (SFJ), 13% (205 limbs) at the saphenopopliteal junction, and 10% (166) in both. Incompetent perforating veins (IPVs) were detected in 1981 limbs, mainly in the SFJ reflux group. The majority of them were direct IPVs as are Dodd, Boyd, Cockett, and paratibial IPV. They were also able to observe a correlation between the prevalence of deep venous reflux and IPVs, especially in the patients in stages C4-6.
Quantification of hemodynamic improvement with
compression stockings, using duplex sonography
B. KAHLE (Germany)
The interest of the authors in measuring femoral volume flow in vein (VFV) and artery (VFA) and the observation of greater values in the varicose vein population has led them to the description of the VAF index which is the ratio of VFV to VFA. They observed values less than 1.00 in the healthy population and superior to 1.4 in the varicose vein population. There was an improvement of these values after surgery. In this study they investigated the effect of compression therapy on the VAF index. They analyzed the results of a group of people before and after (2 hours and 2 weeks) wearing knee- and thigh-length stockings compared with another group wearing no stockings. They observed an improvement in VAF index after compression therapy. These results led them to conclude that the VAF index is a promising tool to measure and quantify the effects of compression therapy.
MANAGEMENT OF CHRONIC VENOUS
INSUFFICIENCY
Chairpersons: J. J. BERGAN (USA), C. ALLEGRA (Italy)
Speakers: P. COLERIDGE-SMITH (UK), A. JAWIEN (Poland),
A. NICOLAIDES (Cyprus), M. A. PISTORIUS (France),
P. SANSILVESTRI-MOREL (France)
During this symposium, some aspects of causation of chronic venous insufficiency (CVI) and their possible treatment were presented.
In discussing epidemiology, Prof Jawien has collected data on problems of venous disorders in the literature and has compared these with results of a recent multicenter cross-sectional study in Poland. There a prevalence of varicose veins, and severe CVI was found to be similar to that in surrounding developed countries. Risk factors including age, family history of varicose veins, obesity, and lack of physical activity were associated with chronic CVI in women more than in men.
There are few studies which have proven the importance of the hereditary factor at a clinical level. In an original study by Dr Pistorius to identify one or several mutations predisposing to varicose vein disease, two families have been identified and examined. This has led to determining the complete genotype of each individual within a family in order to identify new loci of interest. A potential locus has been identified, and further research is focusing on the sequencing of potential genes as well as analysis of new, large families.
Further investigations to study CVI have sought to verify whether the modified collagen composition observed in varicose veins can be reproduced in in vitro cultures. The hypothesis is that CVI may be a systemic disease. In fact, the abnormal collagen accumulation observed in cultures of smooth muscle and dermal cells suggests that indeed, varicose veins could be a systemic disease with a genetic etiology.
It is accepted that abnormalities in the microcirculation contribute heavily to the etiology of varicose veins as well as the chronic skin changes of CVI. Work on animal models has shown that micronized purified flavonoid fractions modulate leukocyte adhesion and prevent endothelial damage. These observations may explain the effect of such flavonoids on management of edema and other symptoms of venous insufficiency. Several studies have demonstrated that from the earliest stages of CVI, MPFF relieves symptoms of pain, paresthesia, and restless legs as well as edema. It decreases bradykinin-induced micro-vascular leakage and inhibits leukocyte activation, trapping, and migration. Now, it has been concluded that this is a first -line treatment for edema as well as other symptoms of CVI. It continues to be effective in all subsequent stages of the disease, including leg ulceration.
In summary this symposium provided an introduction to some of the most promising fields of venous research.
Chairpersons: J. J. BERGAN (USA), E. O. BRIZZIO (Argentina),
P. COLERIDGE SMITH (UK)
Influence of pregnancy and hormones on venous
diseases – results from the Bonn vein study
E. RABE (Germany)
The data from the Bonn study, a cross-sectional study conducted with the support of the German Ministry of Health, are the results of the first epidemiological study conducted in Germany after the Tubingen study of 1979.
More than 3000 people, selected via random sampling, were interviewed using a standardized questionnaire concerning general health and phlebological issues, and were examined clinically and with duplex scanning.
According to the CEAP classification, patients without any venous disease (C0) constituted 9.6%, C1 patients 59.1%, C2 14.3%, C3 13.4%, C4 2.9%, C5 0.6%, and finally C6 0.1%.
The incidence of venous disease was similar in the two sexes, and only in the C2 – C3 classes was there increased prevalence in females.
General risk analysis showed that being overweight is a risk factor for developing chronic venous insufficiency, but not for the presence of varicose veins, and that a lower social class correlates with the presence of chronic venous insufficiency.
The participants were questioned on the number of pregnancies and hormone use, both as oral contraceptives and as hormone replacement therapy. Logistic regression has shown that there is a relationship between the number of pregnancies and the risk of varicose veins.
The odds ratio changes from 1.5 for women with one or two pregnancies, to 1.9 for three, to 2.1 for four, up to an odds ratio of 2.8 for females with 5 or more pregnancies.
While the risk for telangectasias, reticular veins, and varicose veins increases with the number of pregnancies, this effect is less severe for chronic venous insufficiency.
On the contrary, even if the data are less powerful, the use of hormones showed a slight reduction in the incidence of chronic venous insufficiency(CVI) with an odds ratio of 0.4.
It remains to be determined if there is any difference in lowering the risk of CVI between oral contraceptives and hormone replacement therapy.
The incidence of venous disease in Brazil based on the CEAP
classification – an epidemiological study
A. SCUDERI (Brazil)
Dr Scuderi reported on the occurrence of venous disease in the region around Sao Paulo, one of the most relevant figures from Brazil.
More than 2100 people attending the University Hospital, excluding patients from the vascular diseases departments, were given a questionnaire and clinical examination, and classified using the CEAP method.
In the male group 66.48% were 0A/0A, that is, without symptoms and without varicose veins, and similar numbers were present in the female group but only in the younger subgroup.
Subjects aged 14 to 22 years, had 46.42% at stage 0A/0A, while considering women 23 to 48 years of age, two – thirds of whom had undergone one or more pregnancy, only 10.43% were at stage 0A/0A. In the oldest group, 49 years and over, less than 5% were free of visible varicose veins and without symptoms, while 62.79% had both varicosities and symptoms.
This study confirms the utility of using the CEAP classification, and shows results similar to those obtained in epidemiological studies in Western countries; venous diseases appear more common in females than in man, age and number of pregnancies are correlated with the presence of the disease, and up to 50% of young women may have altered veins, without symptoms, but suffer aesthetic discomfort.
A meta-analysis of venous leg ulcer healing in prospective
randomized studies using micronized purified flavonoid
fraction
P. GLOVICZKI (USA)
A meta-analysis to evaluate the efficacy of micronized purified flavonoid fraction (MPFF, MPFF at a dose of 500 mg, Servier, France) in addition to conventional treatment for the healing of venous leg ulcers was presented.
In his introduction, P. Gloviczki reminded that more than 1% of adults will suffer from leg ulcers at some time and that the costs associated with the long-term care of these chronic wounds are substantial. In a recent survey performed in the US,1 the number of new patients has been evaluated to 20 556 each year. Twelve per cent of ulcer patients usually require hospitalization. Annual direct costs has been estimated to USD 150 million to 1 billion. These did not included indirect costs (loss of work days, early retirement, reduced quality of life).
Compression therapy remains the cornerstone of management in venous leg ulcer provided the material used (usually, several layers of elastic bandage), 30 to 40 mm Hg, is able to provide sustained pressures, and is correctly applied. Despite these recommendations, not all ulcers are healed. Thus, the question of the benefit of a systemic pharmacotherapy as an adjuvant to standard compression therapy has been studied. MPFF was chosen for its well – known protective effect on the microcirculation. MPFF indeed appears to work by decreasing the interaction between leukocyte and endothelial cells, reducing the capillary increased permeability. It acts by inhibiting expression of endothelial intercellular adhesion molecule-1 (ICAM 1), and vascular cell adhesion molecule (VCAM), as well as surface expression of some leukocyte adhesion molecules (monocyte or neutrophil CD 62 L, CD11B).
The objective of this meta-analysis was to assess the ability of MPFF used in combination with conventional treatment (ulcer management and compression) in improving the process of venous leg ulcer healing.
Seven comparable, prospective, randomized, controlled studies were identified from medical literature databases and from the files of the manufacturer in which 723 patients with venous ulcers were treated with MPFF (2 tablets daily) or placebo for at least 2 months (1 study) and up to 6 months (4 studies). The percentage of patients with complete healing of the reference ulcer at 6 months was taken as the primary end -point. Secondary end-points consisted of: time to healing after in clusion (in days), rate of complete healing at month 2 and month 4 (% patients completely healed), reduction of reference ulcer area (in % of healed surface), and decrease in associated symptoms (% patients without heaviness and pain).
When compared with controls, ulcer healing at 6 months was in favor of MPFF (61.3% vs 47.7%; RR: 1.32; CI: 1.03-1.70; P=0.03). This was significant from month 2 (RR =1.44, CI=1.07-1.94; P=0.015), and associated with shorter time to healing (P=0.0034), greater reduction of ulcer area (P=0.016 and 0.005 at months 4 and 6 respectively), and greater improvement in symptoms (P<0.005 at months 2, 4, and 6).
These results, along with those of previous individual randomized, controlled trials, confirm that MPFF accelerates the process of venous leg ulcer healing.
Constitutional functional venopathy
C. ALLEGRA (Italy)
Starting from a clinical approach, and listening to patient complaints, the authors focalized on a group of symptoms, which in their view constitute a new clinical entity.
Out of more than 4000 patients studied annually, about a quarter presented with leg discomfort without visible varicose veins, or reflux in the superficial or deep venous system.
These patients presented with a group of symptoms which mainly include edema, heavy legs, subcutaneous fat “cellulite,” acral hypothermia, menstruation irregularities, and blood pressure values at the lower limit of normal.
In addition to clinical and ultrasound methods, a subgroup of patients were also assessed with capillaroscopy, blood samples for hormonal studies, microlymphography, and laser Doppler. A significant decrease in progesterone and a significant increase in prolactin were documented, while microcirculatory investigations showed venular hypertension, microlymphatic overload, and a prepuberal capillaroscopic picture, leading to a decreased venous tone, even in the absence of reflux.
The diameter of the saphenous junction in clino and orthostatism showed an increase of 4.2 mm. The hormonal disturbances could account for the edema, menstrual disturbances, and subcutaneous adipose tissue alterations, and the microcirculatory findings could explain the venous symptoms without venous reflux.
These patients, if correctly identified, could improve with modification of their lifestyle, and with the use of venoactive drugs.
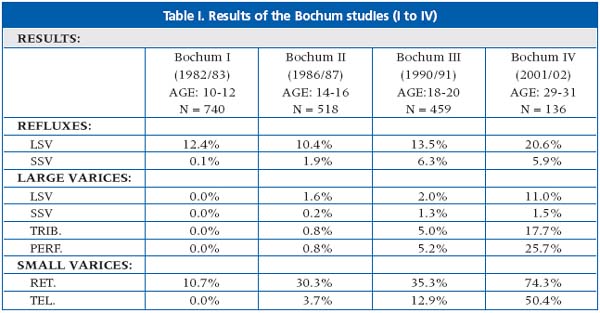
Prospective epidemiological study of developing varicose
veins over a period of two decades (Bochum Study I-IV)
U. SCHULTZ-EHRENBURG (Germany)
The Bochum studies investigated the preclinical and early stages of venous disease, examining a group of students from secondary schools, starting at the ages of 10 to 12 years, and following a group of them up to the age of 29 to 31 years.
The subjects were examined with a questionnaire, measurements, physical exam, photoplethysmography, Doppler ultrasound, and, for the Bochum IV study, with Duplex Scanner.
The results are summarized in Table I.
Even if the decrease in the number of subjects studied, especially in the Bochum IV study, could lead to some selection bias, the study has shown that while reticular varices are present at an early age, telangectasias become apparent later and increase with age.
Varicose veins were essentially present in the Bochum IV study, but reflux in the saphenous vein was present far ahead of visible varices. Females presented with more telangectasias and reticular varices, but tributaries and incompetent perforators were more frequent in men.
A hereditary trait was shown, with all types of varices and reflux that correlated with a positive family history.
The increase of the prevalence is -age and-growthrelated.
The ultrasound detection of reflux usually precedes the clinical appearance of varicose veins, and offers opportunities for preventive measures.
Photoplethysmography did not appear suitable for early detection of venous disease.